Your digestive health, also known as gut health, is intimately related to other aspects of your well-being, such as nervous system function via the gut-brain axis (7) and immune function via the mucosal immune system in the gastrointestinal tract. (3) If you’ve experienced digestive issues, you likely already recognize the importance of a healthy digestive system to your overall health and quality of life.
Understanding how your digestive system works and the factors that can impair digestive health can empower you to alleviate digestive issues.
Understanding the digestive system
The human digestive system is responsible for digesting the foods and beverages you consume into substances that are absorbed by the gastrointestinal tract (GI tract) and used by the body. Digestion involves various mechanical and chemical processes that occur in different parts of the digestive system. (16)
Digestive system anatomy
The digestive system is composed of the hollow organs of the GI tract, including the:
- Mouth
- Esophagus
- Stomach
- Small intestine
- Large intestine
- Anus (15)
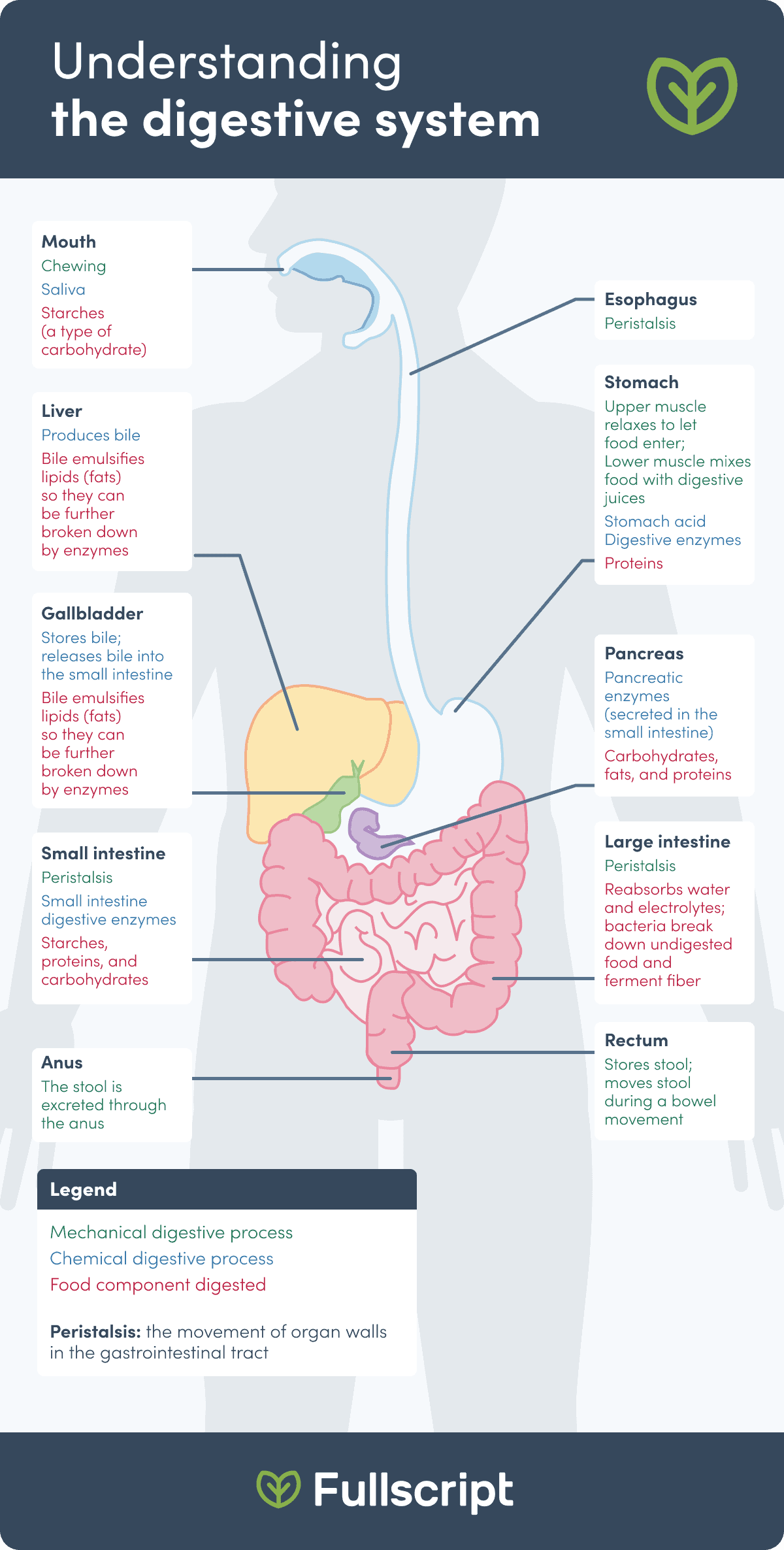
Additionally, the liver, pancreas, and gallbladder are accessory digestive system organs that support the breakdown of food material by secreting chemical substances, such as digestive enzymes and bile. (15) The following digestive system diagram illustrates the organs found within the digestive system and their roles.
Beyond the digestive system organs, digestion relies on various hormones, gut microbiota, the circulatory system, and the enteric nervous system (nerves found within the GI tract). (10)(15) The gut microbiota, which is the community of microbes residing in the human digestive system, deserves particular attention for its various roles in digestive health, including:
- Assisting in nutrient metabolism and absorption
- Maintaining gut barrier function
- Protecting against pathogenic microbes
- Regulating gastrointestinal development (17)
Did you know? The term dysbiosis refers to having a disrupted gut microbial community, which can involve an imbalance of microbial strains and decreased overall microbial diversity. (6)(7)(17)
Digestive system function
The purpose of digestion is to break down the foods and beverages that you consume into smaller components, which provide your body with the macronutrients, micronutrients, and energy it needs to function and maintain health. (15)
Digestion is said to begin even before the ingestion of a meal, as food preparation and anticipation stimulate the secretion of saliva and digestive chemicals in the stomach. Ingesting, chewing, and swallowing food will begin a cascade of steps as the food progresses through the digestive system. (12)
The digestive system is made up primarily of smooth muscle tissues, which act to contract and relax. A process known as peristalsis, this movement of muscles in the hollow organ walls, pushes food through the GI tract. Mechanical processes, such as squeezing and mixing, help to physically break down food into smaller particles and mix food with digestive secretions in the stomach and small intestine. (15)
Chemical processes involve digestive secretions such as stomach acid, bile, and digestive enzymes, which further degrade these food particles into absorbable forms. These digestive secretions are produced and/or released by the stomach, small intestine, liver, gallbladder, and pancreas. (15)
Digestion results in simple sugars (e.g., glucose, fructose and galactose) from carbohydrates, fatty acids and glycerol from fats, and amino acids from proteins. Absorption of these and other substances, such as vitamins, minerals, and water, occurs primarily in the small intestine, followed by their distribution throughout the body by the circulatory system. (15)
Bacteria found in the large intestine produce certain nutrients, such as vitamin K, and ferment remaining undigested nutrients in the colon, such as fibers and proteins. (7) The large intestine absorbs water and transforms toxins and waste products from digestion into stool, which is eliminated during a bowel movement. (15)
Digestive issues
There are a broad variety of digestive issues, ranging from occasional symptoms to chronic digestive system diseases. In general, symptoms of digestive issues include:
- Abdominal pain
- Appetite loss
- Bloating
- Constipation
- Diarrhea
- Fecal incontinence
- Flatulence
- Food intolerance
- Heartburn
- Nausea
- Vomiting
- Weight loss (3)
Functional gastrointestinal disorders
Functional gastrointestinal disorders are a group of conditions characterized by several abnormalities that contribute to digestive issues, such as disturbed motility, increased inner organ pain sensitivity, modified gut microbiota, and altered immune and nervous system function. (8) Functional GI disorders include conditions such as dysphagia, functional constipation, functional dyspepsia, gastroesophageal reflux disease (GERD), and irritable bowel syndrome. (9)
Did you know? Due to dysregulation of the gut-brain axis in functional GI disorders, they’re sometimes referred to as disorders of gut-brain interaction. (5)
1. Dysphagia
Commonly known as difficulty swallowing, dysphagia can occur due to functional changes that affect swallowing or transporting ingested food through the esophagus. (9)
2. Functional constipation
Constipation is a functional disorder characterized by reduced bowel movement frequency and feelings of incomplete and difficult evacuation. (9)
3. Functional dyspepsia
Functional dyspepsia is characterized by recurring or persistent upper abdominal symptoms, such as early feeling of fullness and epigastric (upper abdomen) pain and/or burning. (9)
4. Gastroesophageal reflux disease
Gastroesophageal reflux disease (GERD) is sometimes used interchangeably with acid reflux; however, GERD is a more complex condition characterized by impaired esophageal peristalsis, food transit, esophageal sphincter function, and stomach emptying. Symptoms of GERD include belching, and feeling acidity, burning, and pain in the chest. Some individuals also experience coughing, hoarse throat, and asthma. (9)
5. Irritable bowel syndrome
A chronic functional GI disorder, irritable bowel syndrome (IBS) is characterized by irregular bowel habits and recurring abdominal pain. Individuals with IBS may experience primarily symptoms of constipation (IBS-C), diarrhea (IBS-D), mixed symptoms (IBS-M), or varied/undetermined symptoms (IBS-U). (1)
Did you know? IBS is a common condition, affecting an estimated 5 to 15% of individuals in Western countries. (1)
Digestive system diseases
There are a variety of other gastrointestinal diseases that are not a result of functional changes in the digestive system. Instead, these conditions may occur due to certain infections or irregular inflammation and immune system responses. (7)(9)
1. Atrophic gastritis
A chronic inflammatory condition, atrophic gastritis is characterized by inflammation of the stomach’s mucosa (mucous membrane layer). Atrophic gastritis has been associated with reduced stomach acid secretion, malabsorption of several nutrients (e.g., calcium, iron, vitamin B12), and increased risk of Helicobacter pylori infection and dyspepsia. (9)
2. Inflammatory bowel diseases
Crohn’s disease and ulcerative colitis are the two primary inflammatory bowel diseases (IBDs). While both conditions are chronic relapsing diseases, Crohn’s disease may affect the entire organ wall of any part of the GI tract, and ulcerative colitis affects only the mucosa and submucosa layers of the colon. (2)
3. Liver diseases
There are a number of different liver diseases, such as chronic hepatitis, cirrhosis, and hepatocellular carcinoma. (9) Liver diseases may be caused by viruses, as in viral hepatitis, or by environmental toxins, such as drug use and excessive alcohol intake. (13)
4. Pancreatitis
Inflammation of the pancreas, known as pancreatitis, can be acute (short-term) or chronic (long-term). This condition may result from different factors, such as gallstone formation and the accumulation of environmental toxins in the body. (9)
5. Peptic ulcer disease
Peptic ulcers, commonly called stomach ulcers, are characterized by the formation of sores on the lining of the stomach or the duodenum (first section of the small intestine), causing burning or dull pain in the stomach. Having an H. pylori infection and chronically taking nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin and ibuprofen, can increase your risk of peptic ulcer disease. (14)
Causes and risk factors for digestive issues
Many factors may contribute to one or more digestive issues, such as:
- Certain conditions (e.g., anxiety, depression, diabetes, hypothyroidism, multiple sclerosis, myopathies, Parkinson’s disease)
- Certain medications (e.g., antacids, antibiotics, anticholinergics, antidepressants, antihistamines, antihypertensives, NSAIDs, opioids) (3)(9)
- Chronic stress (3)(7)
- Colorectal disorders (e.g., colonic stenosis, hemorrhoids, fissures) (9)
- Environmental toxins (e.g., air pollution) (7)
- Inactivity or excessive strenuous exercise (2)(3)
- Insufficient hydration (11)
- Poor dietary habits (e.g., chronic/excessive intake of alcohol, (4) carbonated beverages, large meals, (9) saturated fats, (7) insufficient dietary fiber) (6)
- Sleep disorders and/or insufficient sleep (10)
- Smoking (9)
Certain physiological changes that normally occur during aging may result in decreased digestive system function. These changes include altered food swallowing, reduced peristalsis of the esophagus, and decreased digestive secretions (e.g., gastric acid, pepsin, pancreatic enzymes, bile salts). (9) It’s best to speak to your integrative healthcare practitioner if you’re experiencing digestive problems.
The bottom line
The digestive system, composed of a variety of primary and accessory digestive system organs, is responsible for the breakdown and absorption of dietary components, as well as the excretion of toxins and waste products. Several environmental and lifestyle factors may impair your digestive health and increase your risk of digestive issues. If you’re a patient experiencing digestive issues, consider making changes to support your digestive health and consult with your integrative healthcare practitioner for guidance.
- Alammar, N., Wang, L., Saberi, B., Nanavati, J., Holtmann, G., Shinohara, R. T., & Mullin, G. E. (2019). The impact of peppermint oil on the irritable bowel syndrome: A meta-analysis of the pooled clinical data. BMC Complementary and Alternative Medicine, 19(1), 21.
- Bilski, J., Mazur-Bialy, A., Brzozowski, B., Magierowski, M., Zahradnik-Bilska, J., Wójcik, D., Magierowska, K., Kwiecien, S., Mach, T., & Brzozowski, T. (2016). Can exercise affect the course of inflammatory bowel disease? Experimental and clinical evidence. Pharmacological Reports, 68(4), 827–836.
- Bischoff, S. C. (2011). “Gut health”: A new objective in medicine? BMC Medicine, 9(1), 24.
- Bishehsari, F., Magno, E., Swanson, G., Desai, V., Voigt, R. M., Forsyth, C. B., & Keshavarzian, A. (2017). Alcohol and Gut-Derived Inflammation. Alcohol research : current reviews, 38(2), 163–171.
- Black, C. J., Drossman, D. A., Talley, N. J., Ruddy, J., & Ford, A. C. (2020). Functional gastrointestinal disorders: Advances in understanding and management. The Lancet, 396(10263), 1664–1674.
- Chiba, M., Ishii, H., & Komatsu, M. (2019). Recommendation of plant-based diets for inflammatory bowel disease. Translational Pediatrics, 8(1), 23–27.
- Conlon, M., & Bird, A. (2014). The impact of diet and lifestyle on gut microbiota and human health. Nutrients, 7(1), 17–44.
- Drossman, D. A. (2016). Functional gastrointestinal disorders: History, pathophysiology, clinical features, and rome IV. Gastroenterology, 150(6), 1262–1279.e2.
- Grassi, M., Petraccia, L., Mennuni, G., Fontana, M., Scarno, A., Sabetta, S., & Fraioli, A. (2011). Changes, functional disorders, and diseases in the gastrointestinal tract of elderly. Nutricion hospitalaria, 26(4), 659–668.
- Khanijow, V., Prakash, P., Emsellem, H. A., Borum, M. L., & Doman, D. B. (2015). Sleep Dysfunction and Gastrointestinal Diseases. Gastroenterology & hepatology, 11(12), 817–825.
- Liska, D., Mah, E., Brisbois, T., Barrios, P. L., Baker, L. B., & Spriet, L. L. (2019). Narrative review of hydration and selected health outcomes in the general population. Nutrients, 11(1), 70.
- Livovsky, D. M., Pribic, T., & Azpiroz, F. (2020). Food, eating, and the gastrointestinal tract. Nutrients, 12(4), 986.
- National Institute of Diabetes and Digestive and Kidney Diseases. (2021a). Liver Disease. https://www.niddk.nih.gov/health-information/liver-disease
- National Institute of Diabetes and Digestive and Kidney Diseases. (2021b). Peptic ulcers (stomach ulcers). https://www.niddk.nih.gov/health-information/digestive-diseases/peptic-ulcers-stomach-ulcers
- National Institute of Diabetes and Digestive and Kidney Diseases. (2021c). Your digestive system & how it works. https://www.niddk.nih.gov/health-information/digestive-diseases/digestive-system-how-it-works
- Patricia JJ, Dhamoon AS. Physiology, Digestion. . In: StatPearls . Treasure Island (FL): StatPearls Publishing; 2021 Jan-. https://www.ncbi.nlm.nih.gov/books/NBK544242/
- Swallah, M. S., Yu, H., Piao, C., Fu, H., Yakubu, Z., & Sossah, F. L. (2021). Synergistic Two-Way interactions of dietary polyphenols and dietary components on the gut microbial composition: Is there a positive, negative, or neutralizing effect in the prevention and management of metabolic diseases? Current Protein & Peptide Science, 22, 313–327.